Glaucoma is a progressive eye disease of the optic nerve often caused by increased intraocular pressure (IOP).
GLAUCOMA
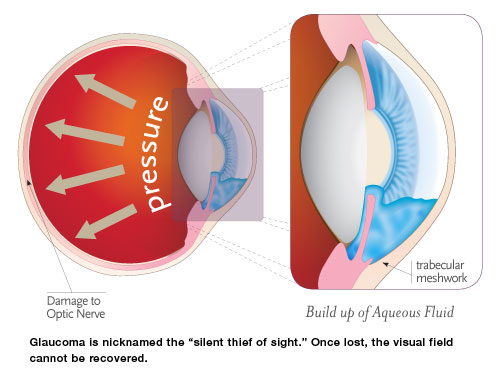
Increased IOP results either from a malfunction of the eye’s drainage structures or from increased production of fluid inside the eye (aqueous humor). Left untreated, elevated IOP can cause irreversible damage to the optic nerve and retinal fibers, resulting in a progressive, permanent loss of vision. However, not all cases of glaucoma are related to increased IOP. In fact, studies have shown that up to one-third of patients with glaucoma will have IOP in the normal range at an annual eye exam. Early detection and treatment can slow or even halt the progression of the disease.
-
What Causes Glaucoma?
The eye constantly produces aqueous, the clear fluid that fills the anterior chamber (the space between the cornea and iris). The aqueous filters out of the anterior chamber through a complex drainage system. The delicate balance between the production and drainage of aqueous determines the eye’s IOP.
After nourishing the cornea and lens, the fluid flows out through a very tiny spongy tissue called the trabecular meshwork, which serves as the drain of the eye. When this drain becomes clogged, fluid cannot leave the eye as fast as it is produced. This causes the fluid to back up, which in turn causes increased pressure build up within the eye.
When the pressure in the eye builds, the nerve cells that make up the optic nerve and their blood supply become compressed, causing them to become damaged and eventually die. The death of these cells results in permanent visual loss. Early diagnosis and treatment of glaucoma can prevent this from happening.
-
What Are the Different Types of Glaucoma?
There are two major types of glaucoma: primary open-angle and closed-angle glaucoma.
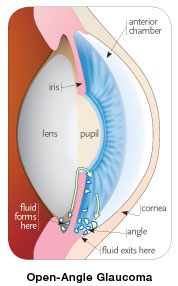
Primary open-angle glaucoma is the most common form of glaucoma. In open-angle glaucoma, the drainage canals in the eyes become clogged gradually over months or years. Pressure in the eye rises slowly because fluid is produced at a normal rate but drains sluggishly. Damage occurs over time, usually without notice.
Closed-angle glaucoma is far less common than open-angle glaucoma. In closed-angle glaucoma, the drainage canals in the eyes suddenly become blocked or covered. Pressure in the eye rises rapidly because fluid drainage is abruptly blocked while production continues. An “attack” may produce a red, painful eye and other symptoms such as facial pain, headache, blurry vision, rainbow-colored halos around lights, nausea and vomiting. It is considered a medical emergency.
Normal-tension glaucoma, also known as low-tension glaucoma, is an open-angle type of glaucoma that can cause visual field loss due to optic nerve damage. This is a unique condition that occurs even though pressure inside the eye is normal. Because of its silent nature, people do not usually have any visual complaints until late in the course of the disease. Often times, a person with normal-tension glaucoma will not notice vision loss until significant amounts of optic nerve damage and permanent vision loss have already occurred.
-
What Are the Symptoms?
At first, there are no symptoms of glaucoma; this disease is known as the “silent thief of sight.” Vision stays normal and there is no pain.
Primary open-angle glaucoma signs and symptoms include:• Gradual loss of peripheral vision (usually in both eyes)
• Tunnel vision in the advanced stages
Closed-angle glaucoma signs and symptoms include:• Eye pain
• Nausea and vomiting (accompanying the eye pain)
• Sudden onset of visual disturbance (often in low light)
• Blurred vision
• Halos around lights
• Reddening of the eye

-
How is Glaucoma Diagnosed?
Early diagnosis, through regular and complete eye exams, is the key to protecting your vision from damage caused by glaucoma. Your surgeon may perform a number of tests to diagnose glaucoma: tonometry (measures your IOP), gonioscopy (inspects the drainage angle of the eye), or visual field (tests the peripheral vision). In addition, careful examination of the optic nerve by your surgeon will be performed and is the most sensitive test for diagnosing glaucoma. Advanced digital imaging technology provides your doctor with additional and sophisticated information about the structure of the optic nerve and assists in the diagnosis and monitoring of glaucoma. New instruments (scanning laser polarimetry [SLP], optical coherence tomography [OCT], and confocal scanning laser ophthalmoscopy) assist your doctor in his or her evaluation.
How Can Glaucoma Be Treated?
A variety of options are available to treat glaucoma, including eyedrops, laser procedures and surgery. All are intended to decrease eye pressure and thereby protect the optic nerve. Currently in the United States, eyedrops or laser are the first choice for treating patients. For many people, a combination of medications and laser treatment can safely control eye pressure and prevent further vision loss.
-
Medications:
Eye drops are used in managing glaucoma to decrease eye pressure. This helps the eye’s fluid drain better and/or decreases the amount of fluid made by the eye. Drugs to treat glaucoma are classified by their active ingredient. These include prostaglandin analogs, beta-blockers, alpha-agonists and carbonic anhydrase inhibitors. In addition, combination drugs are available for patients who require more than one type of medication.
For most people with glaucoma, regular use of medications will control the increased fluid pressure. However, these drugs may stop working over time or may cause side effects. This is one of the reasons why a person with glaucoma must be seen several times a year. If a problem occurs, the doctor may select alternative drugs, change the dose, or recommend other options.
-
Laser Procedures:
Lasers are very useful for treating glaucoma and are increasingly used as a “first-line” treatment in addition to medications. Laser Trabeculoplasty: This is usually done to treat open-angle glaucoma. When performing Laser Trabeculoplasty, the doctor aims the laser at the trabecular meshwork on the inside-front part of the eye. Then the doctor uses the laser to treat 50 to 100 spots on the trabecular meshwork. The laser opens clogged areas and helps eye fluid drain out more easily. The newest form of laser is called selective laser trabeculoplasty (SLT). This state-of-the-art technology has been shown to be repeatable without any damaging effects to the eye. Some patients who have this laser treatment may even be able to stop their eyedrops.
-
Laser Iridotomy:
This is usually done to treat closed-angle glaucoma. This will allow fluid to pass from behind your iris, where it is produced, to the trabecular meshwork, where it can drain.
“IN THOSE PATIENTS WHERE THE PRESSURE CANNOT BE CONTROLLED WITH MEDICATION OR LASER, SURGERY IS OFTEN SUCCESSFUL IN REDUCING IOP.”
Surgery
In those patients whose pressure cannot be controlled with medication or laser, surgery is often successful in reducing IOP. Surgical procedures create a drainage channel in the front part of the eye to help fluid escape. Sometimes, a tube is placed in the eye to facilitate and to help maintain adequate drainage.
What can you do to protect your vision?
Studies have shown that early diagnosis and treatment of glaucoma (before it causes major vision loss) is the best way to control the disease. Once damage from glaucoma occurs it is not reversible. Depending on your general health and family history, your eyes should be examined through dilated pupils every one to two years by your eye doctor. However, if you have glaucoma risk factors, we recommend a dilated eye examination every year.


